In Ghana, Grace Marquis is exploring the relationship between infant health, HIV-positive mothers and breast milk. And it’s not what you think.
By Andrew Mullins

When one thinks about infant mortality due to malnutrition, chances are good that archetypal media image of famine spring to mind: the pictures of children bereft of fat or muscle, the proverbial collection of “skin and bones.” But, according to Grace Marquis, associate professor in the School of Dietetics and Nutrition and the Centre for Indigenous Peoples’ Nutrition and Environment (CINE), such extreme cases actually account for only 17 per cent of child malnutrition deaths in developing countries. It’s mild to moderate malnutrition, she’s learned, that kills more kids. “You look at these children and think they’re perfectly fine,” she says. “For many, their weight may be low but, because they also are stunted—they have a low height for their age—the malnutrition is not so obvious.” This is not the only surprising revelation stemming from Marquis’ current work in Ghana.
A Big RIING
Marquis is collaborating with researchers from the University of Ghana, Iowa State University and the University of Connecticut to study how the HIV status of mothers in eastern Ghana can affect the diet and care of their children. The $1.5-million, five-year Research to Improve Infant Nutrition and Growth (RIING) project is part of a U.S. National Institutes of Health campaign to strengthen the research capacity of sub-Saharan institutions. The RIING team’s findings may eventually save lives and promote healthier childhoods for millions.
The RIING research is ambitious, recruiting 450 mothers from the Manya Krobo district of eastern Ghana. The region has the country’s highest incidence of HIV—around 4.7 per cent—and poverty is the norm. The mothers are equally selected from three groups: HIV-positive, HIV-negative and women of unknown HIV status. Beginning during pregnancy, and lasting until the child turns one year old, the researchers gather painstakingly detailed data. They collect demographic basics (age, sex, education level, occupation) about each occupant, as well as socio-economic information (including indicators of cumulative wealth and notes about the housing’s physical quality). The researchers also monitor the family’s agricultural practices and household food security as defined by the Food and Agriculture Organization. (According to the FAO, “Food security exists when all people, at all times, have physical, social and economic access to sufficient, safe and nutritious food which meets their dietary needs and food preferences for an active and healthy life.”)
Comprehensive Monitoring
The stigma attached to HIV is strong in Ghana. Although there is generally a good understanding about true transmission routes (sexual behaviour, needle sharing, mother-to-child), there remain misconceptions that HIV can be spread through direct contact; religious beliefs, gender biases and notions equating HIV with infidelity also contribute to the confusion. As a result, HIV-positive women risk being kicked out of their houses by their partners or family, losing access to secure living quarters and food for themselves and their children. Researcher-subject confidentially is therefore crucial. The RIING staff stress that the study is related to child growth and health; HIV is never publicly mentioned, and only the field supervisor knows the participants’ health status.
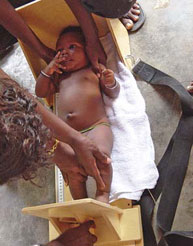
RIING field workers, all women mostly from the region (and fluent in at least one of Manya Krobo’s nine official languages and numerous dialects), visit the households twice weekly to collect information on the health of both mother and child. Once a month they gauge how well the children are growing by measuring weights and heights, and the circumferences of their heads, arms and chests. The team also carefully monitors each child’s diet, tracking daily nutrition and noting whether the child is breastfed or has received water, dairy products or other foods. Every three months, the researchers conduct a 24-hour monitoring of dietary intake, which includes weighing the breastfed child before and after feedings to measure the intake of milk.
The comprehensive monitoring of the women sounds invasive, Marquis admits, “but what we’ve found is that once a mother has participated in the process, the next day they’re asking, ‘When are you coming back?’ The field workers provide a level of companionship and camaraderie that is very attractive to the moms.”
Maximizing Mother’s Milk
Breastfeeding is of particular importance to the researchers. The World Health Organization has recommended that if HIV-positive women do not have access to safe water and can’t afford adequate formula, they should practise exclusive breastfeeding—no water or food other than breast milk—for a full six months. The WHO’s advice may seem to be counterintuitive, notes Marquis, but is medically sound.

“You would think less breast milk from an HIV-infected mother would be better,” she says, “but when you exclusively breastfeed, your child has a healthy gut. When you introduce non-breast-milk foods to young children before the age of six months, you increase the risk of damage to the gut mucosa [the inner lining of the gastrointestinal tract], so the children are more susceptible to infection.” The child’s risk of HIV infection therefore actually decreases when the child is exclusively breastfed by an HIV-positive mother. Further, when this breastfeeding is combined with the drug neveripine during childbirth, and a postpartum regimen of anti-retroviral drugs, the risk of mother-to-child transmission of HIV can be reduced dramatically.
There has been a concerted, nationwide effort by the Ghana Health Services and NGOs working in the area of child health to encourage exclusive breastfeeding and continued breastfeeding with complementary feeding. As a result, Ghana’s overall breastfeeding rate is high: a 2003 national survey reported one-third of mothers exclusively breastfed at six months, and the mean duration of any breastfeeding was 23 months. (In North America, only about 10 per cent of women breastfeed beyond 12 months.) Still, RIING’s preliminary findings indicate that the early breastfeeding practices of HIV-positive women in Manya Krobo remain less than ideal. “They’re more likely to practice mixed breastfeeding—alternating breast milk with traditional porridges such as koko—a corn-based gruel low in energy and nutrients—in comparison to the mothers who are HIV-negative,” says Marquis. “This mixed feeding behaviour is the opposite of that which is recommended because of the increased risk of diarrheal diseases, malnutrition, as well as HIV transmission. So you need to make sure that the message you’re giving about exclusive breastfeeding is reaching those most at risk: your HIV population.”
Giving Back
There is still much data to gather and analyze, and several years before all of the results are available. “Maybe what we’ll find is that food supplementation programs are needed for children of HIV-infected mothers, regardless of the child’s HIV status,” suggests Marquis. “Or it could be that social systems are falling apart and there need to be interventions to support the mothers. It could be that agricultural practices are changing dramatically—as when households choose to produce crops that require less energy to plant and harvest—and mothers need help with that.”
Downloading information back into the community is crucial. Throughout the project, RIING researchers have given periodic updates to the Ghana Health Services, local HIV clinics and the Queen Mothers Association (a local group of traditional women leaders who have worked actively on the problem of HIV). Upon completion, the researchers will also hold a final workshop to inform community leaders, other researchers and program implementers of the study results. Once they are armed with hard data, says Marquis, “governments, NGOs and communities will be able to make decisions about when and how to intervene and provide effective support or training to help all of these families that are affected by HIV.”
Grace Marquis is the Canada Research Chair in Social and Environmental Aspects of Nutrition. The RIING Project is funded by the U.S. National Institutes of Health.
Next: Making Government Work
